Gastric Bypass Surgery
(Roux-en-Y)
The gold standard in bariatric surgery for over 50 years — delivering powerful, lasting weight loss with proven metabolic benefits for patients across South Texas.
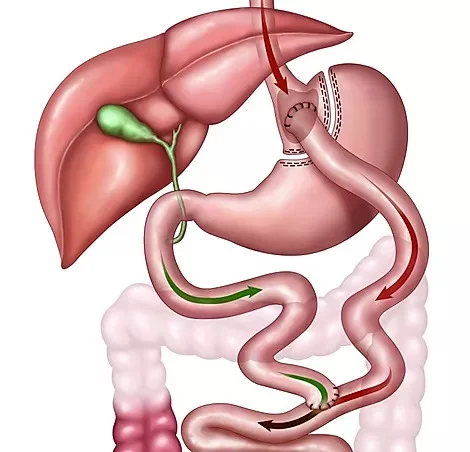
What Happens During Gastric Bypass
The Roux-en-Y Gastric Bypass works in two ways simultaneously: restriction and malabsorption. First, the stomach is divided to create a small pouch — roughly the size of an egg — which severely limits how much food you can eat at one time. Second, the small intestine is rerouted so food bypasses the larger stomach and the first section of the intestine, reducing calorie and nutrient absorption.
This combination triggers powerful hormonal and metabolic changes — particularly in hunger-regulating hormones like ghrelin — that go far beyond simple restriction. Patients lose significantly more weight than diet and exercise alone could ever achieve.
Powerful hormonal & metabolic reset
The intestinal bypass creates gut hormone changes that dramatically boost weight loss beyond what restriction alone provides.
Significant improvement of diabetes
~75% of Type 2 diabetes patients see full remission — often before they've even lost significant weight.
Resolves acid reflux / GERD in 90%+ of patients
Gastric bypass is the preferred procedure when severe reflux is present — it resolves GERD better than any other bariatric surgery.
Enforces better eating habits naturally
Many patients find that foods high in sugar or fat cause discomfort — which naturally reinforces healthier dietary choices over time.
50+ years of long-term outcome data
The most thoroughly studied bariatric procedure in the world — patients and surgeons have decades of real-world evidence to draw from.
Dietary Changes & What to Expect After Surgery
Gastric bypass creates real and lasting changes to how your body processes food. Understanding these upfront helps you prepare for long-term success.
Sugar sensitivity — "Dumping Syndrome"
Eating foods with more than ~10g of sugar at once can trigger dumping syndrome — sweating, rapid heartbeat, cramping, and nausea lasting 20–30 minutes. While uncomfortable, many patients find this actually helps them avoid sugary foods long-term.
Greasy foods cause nausea
High-fat, greasy foods frequently cause significant nausea after gastric bypass. This is a natural reinforcement mechanism that encourages a lower-fat diet — one of the keys to long-term success.
Possible lactose intolerance
Many patients develop lactose sensitivity after bypass — milk, ice cream, and other dairy products in larger amounts may cause discomfort. Lactose-free alternatives and smaller portions are usually well-tolerated.
Daily vitamin supplements required for life
Because the bypass reduces nutrient absorption, patients must take a daily multivitamin, calcium, vitamin B12, iron, and vitamin D for the rest of their lives. Our dietitian team helps you build a supplement routine that works.
Regular lab work & follow-up care
Annual blood work monitors nutritional status, vitamin levels, and metabolic health. Our program provides lifelong follow-up for every patient — because your success doesn't end at surgery.
Alcohol absorption changes significantly
After bypass, alcohol is absorbed much faster and the effects are more intense. Patients are counseled on responsible alcohol use, and we screen carefully for alcohol dependency both pre- and post-operatively.
Understanding Dumping Syndrome
Dumping syndrome occurs when food moves too quickly from the stomach pouch into the small intestine — typically triggered by sugary or high-fat foods. Symptoms include sweating, rapid heartbeat (tachycardia), severe abdominal cramping, and nausea, usually lasting 20–30 minutes.
While not dangerous, dumping syndrome is very uncomfortable — and for many patients, that discomfort becomes a powerful deterrent against high-sugar foods. A small amount of sugar is usually fine (e.g., a single chocolate kiss), but a full candy bar would likely trigger symptoms. This natural feedback mechanism is one of the reasons gastric bypass is so effective at changing eating behaviors long-term.
Who Is the Ideal Gastric Bypass Candidate?
Gastric bypass is an excellent choice for many patients — particularly those with certain health conditions where it outperforms other procedures. Here's what makes someone a strong candidate:
BMI of 35–55+ — effective across a wide range of BMI levels
Severe acid reflux / GERD — bypass resolves reflux in 90%+ of patients, making it the preferred procedure when reflux is a major concern
Type 2 diabetes — ~75% remission rate, often before significant weight loss
High blood pressure, high cholesterol — both improve significantly after bypass
Failed prior weight loss attempts — including other diets, medications, or programs
Committed to lifelong follow-up — supplements, labs, and dietary changes
BMI 50+ — the duodenal switch or SADI-S typically delivers superior weight loss at very high BMIs
Lower surgical risk preference — the gastric sleeve is technically simpler with no intestinal connections
History of inflammatory bowel disease — may increase risk of complications with intestinal rerouting
Unable to commit to daily supplements — nutritional deficiency is a real risk without consistent supplementation
Every case is unique. Our surgeons evaluate each patient individually — the right procedure for you depends on your BMI, health conditions, anatomy, and goals. Schedule a consultation to discuss your best option.
Gastric Bypass vs. Other Procedures
See how gastric bypass stacks up against other surgical weight loss options available at Better Weigh Center in Corpus Christi.
| Factor | Gastric Bypass | Gastric Sleeve | SADI-S | Duodenal Switch |
|---|---|---|---|---|
| Excess Weight Loss | 65–75% | 60–70% | 80–85% | 80–90% |
| Diabetes Remission | ~75% | ~60% | ~90% | ~95% |
| Resolves Acid Reflux | ✓ Yes (90%+) | May worsen | Mostly yes | Mostly yes |
| Intestinal Bypass | Yes | No | Yes (~50%) | Yes (~75%) |
| Hospital Stay | 2–3 days | 1–2 days | 2–3 days | 2–4 days |
| Long-term Data | 50+ years | ~15 years | ~6 years | 20+ years |
| Ideal BMI | 35–55+ | 35–50 | 40+ | 50+ |
Ready to Learn If Gastric Bypass Is Right for You?
Our board-certified bariatric surgeons in Corpus Christi will evaluate your individual history, health conditions, and goals — and give you an honest recommendation on the best path forward.
Serving Corpus Christi, South Texas, Victoria, Laredo, McAllen & surrounding areas
